The entire healthcare industry is waking up to the importance of focusing on outcomes, so it shouldn’t be surprising that physical care environments would be exempt. We’re living in a period where the rooms, offices, and facilities where so much of the healthcare process takes place are being examined for the impact they have on care and medical outcomes.
This is where the world of evidence-based design starts, and that’s one that anyone interested in keeping up with the hospital of the future should make an effort to understand.
What is Evidence-Based Design?
Instead of basing the design on aesthetics or functionality, evidence-based design (EBD) roots decisions on research which contribute to optimal outcomes. EBD is grounded on the idea that physical environments can impact things like patient and staff safety, quality of care, and productivity. It might sound abstract, but you’ve likely seen it before. Think of things like continuous handrails leading to a toilet or decentralized nurse stations that make access to supplies easier.
There are eight steps involved in converting evidence into healthcare environments that contribute to excellent outcomes.
- Defining goals and objectives
- Identifying and finding sources for relevant evidence
- Interpreting that evidence from a critical perspective
- Creating and innovating the required evidence-based design concepts
- Developing a hypothesis
- Collecting baseline performance measures
- Monitoring the implementation of design and construction
- Measuring post-occupancy performance results
It’s worth remembering that, while EBD is applied to many fields, it finds its roots in healthcare, being born out of Robert Ulrich’s 1984 study, View through a window may influence recovery from surgery.
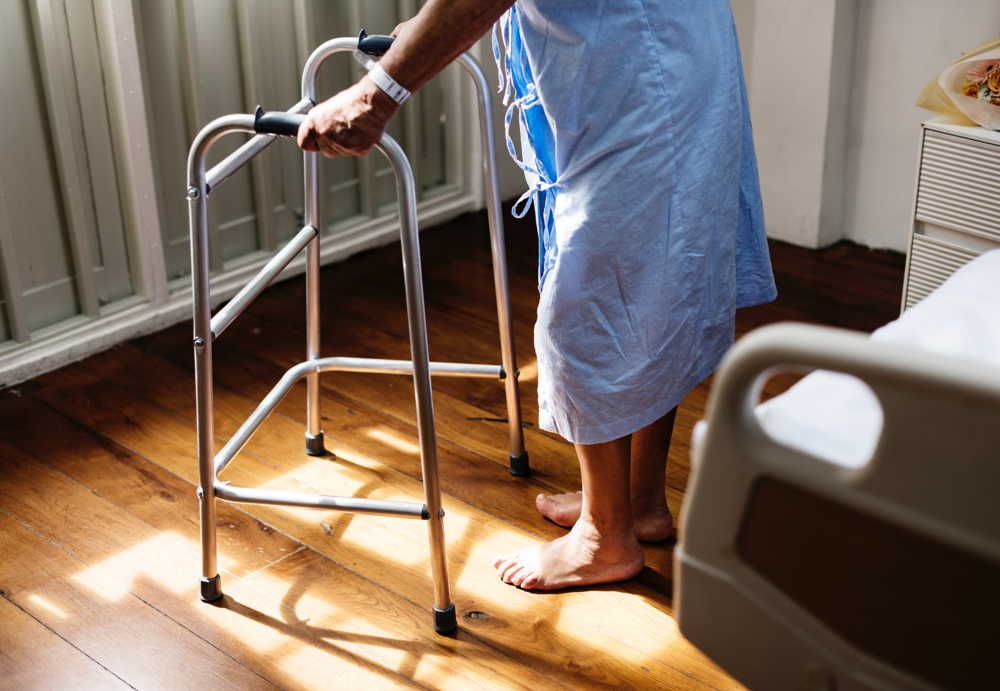
Since that study, the field has evolved considerably to included dedicated journals, long-term efforts like the Pebble Project (intended to create rippling change across the industry), and even works that question and disprove particular beliefs in the field (like the idea that specific colors encourage outcomes.)
EBD Advantages That Can’t Be Ignored
Since evidence-based design has such a long history in the industry, we have a pretty solid idea of the advantages it offers. Some of these advantages include:
A Simpler Design Process
The structured nature of the EBD process means that teams can identify goals and criteria more quickly. It also means coordination among multi-disciplinary teams is easier, opening the chance of discovering design opportunities along the way.
Saved Time
The healthcare facility design process can be long and involved, but, having set goals and research-based best practices increase efficiency. These practices cut back on meetings and grant stakeholders more time to do their actual jobs. The result is a project that not only runs smoothly but is also more likely to meet deadlines.
Risk Avoidance
Healthcare design decisions can be permanent or entail a high cost to change. Implementing the best practices inherent in EBD means that decisions are made based on tested hypotheses. These practices decrease risk and unnecessary loss of time and money.
Improved Operations
The final result of a healthcare environment built on evidence-based principles is one that improves workflows. All those factors work together to improve the day-to-day operations of a hospital and decrease operating costs over time.
New knowledge is continually being created in the field of EBD. This means benefits we see today will continue evolving to meet the needs of the industry and individual care communities.
Is EBD Worth it?
Discussing advantages is one thing, but even with all the proof around them, is investing in EBD worth it? Let’s take a look at some of the more concrete benefits an evidence-based approach provides to hospitals.
Something as simple as the use of natural light can make a big difference, and EBD implementations have demonstrated an ability to impact patient’s use of medication. According to researchers at The Center of Health Design, natural light can decrease medication costs by 21 percent. Additionally, having a view of the outdoors can improve positive emotions and reduce pain. A drop in medication consumption is connected to faster discharges and maximized reimbursement potential. This dynamic is especially important for facilities which are adjusting to new value-based care reimbursement structures.
From another perspective, hospital worker injuries alone rack up a startling $2 billion in worker compensation each year, and many are preventable. For example, Sacred Heart Medical Center at RiverBend in Springfield, Oregon implemented ceiling lifts to aid in transferring patients and virtually eliminated injuries from patient handling. The administration believes the lifts paid for themselves within two years because of the drop in worker’s compensation claims.
Perhaps most interesting though, is the use of small, locked cabinets in patient rooms as a part of a decentralized medication storage plan that had a direct impact on medical errors. Clarian Health Partners implemented EBD changes within its ICU by using adaptable rooms in which in-room storage areas only contained medications for individual patients. The result? An almost 70 percent decrease in medication errors. In addition, Clarian Health Partners had a 90 percent reduction in transfers because of the new room design.
Getting Started on Your EBD Plan
Considering the direction of the industry, every healthcare facility should be open to implementing at least some principles of EBD. Making the right start though is critical.
We’ve discussed the eight-step process, but it’s even more important to prepare your staff for implementation. Make sure that you’re engaging stakeholders as early in the process as possible, and taking the time to build a diverse team that includes not only architectural and construction professionals, but also designers, patients, caregivers, facilities operations, advocacy groups, and support services professionals on top of the C-suite.
Most importantly though, maintain a focus on value that will help you build a dynamic hospital ready to face challenges in the future of healthcare. To learn how cabinet-level access control can strengthen your EBD plan, visit our Healthcare Access Control page.






